
Pregnant woman sitting at kitchen table with laptop and documents reviewing Medicaid application options
Pregnancy Medicaid Eligibility and Benefits Guide
Content
Finding out you're pregnant brings excitement—and questions about healthcare costs. Nearly half of all births in the United States receive Medicaid coverage. If you're worried about affording prenatal visits, ultrasounds, or hospital delivery, you're not alone, and there's help available.
The good news? Income limits for pregnant women are substantially higher than regular Medicaid thresholds. You might qualify even with a full-time job and steady paycheck. This guide walks through exactly how pregnancy Medicaid works, what income your state allows, how to navigate the application, and what happens after your baby arrives.
What Is Pregnancy Medicaid and Who Qualifies
Think of pregnancy Medicaid as a fast lane into comprehensive health coverage. States treat pregnancy as a special category because early prenatal care prevents complications, reduces premature births, and improves outcomes for both mothers and babies.
Here's what makes it different: while regular adult Medicaid in many states only covers people below poverty level (or not at all), pregnancy opens doors to Medicaid for households earning twice that amount or more. A family of three making $60,000 annually might still qualify in some states.
The "presumptive eligibility" rule matters tremendously. Walk into certain clinics and health centers, provide basic income information, and you can receive temporary Medicaid on the spot—sometimes within an hour. This temporary coverage lasts while your full application processes, typically 30 to 60 days. No more postponing that first appointment because you're unsure about costs.
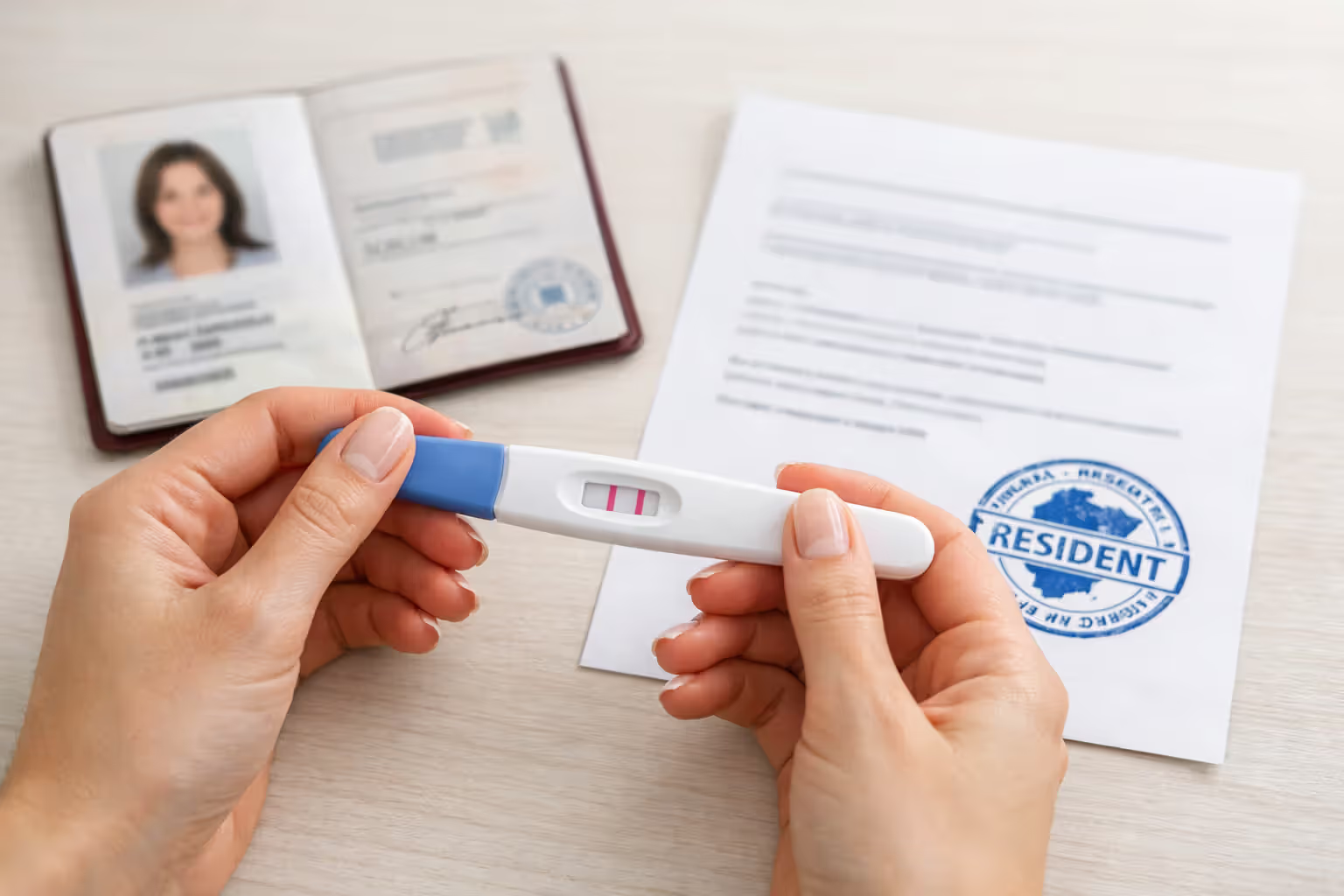
Three things determine whether you're eligible: you need confirmation of pregnancy (a positive test works), income within your state's limits, and residency in that state. Immigration status plays a role, though requirements have loosened over time. Most states now cover pregnant women with legal immigration status, regardless of how recently they arrived. Several states go further, using state dollars to cover prenatal care for undocumented residents.
Author: Derek Whitmore;
Source: blaverry.com
One surprise for many applicants: pregnancy Medicaid for adults means exactly that—any pregnant person qualifies regardless of age. Whether you're 19 or 42, with your first baby or your fifth, pregnant and within income limits equals eligible.
A common question: "I'm only four weeks along—should I wait to apply?" No. Apply now. Processing takes time, and you want coverage active before that first appointment around week 8 or 10.
Income Limits and Financial Requirements by State
Federal rules require states to cover pregnant women earning up to 138% of the poverty line at minimum. In practice, most states blow past that floor. Finding a state that only covers the minimum is actually harder than finding one offering 200%, 250%, or even 300% of poverty level.
What does that mean in real dollars? The 2026 federal poverty level for a three-person household sits around $25,820 per year. Now double that—$51,640 annually—and you're at 200% of poverty level. Many working families fall into this range.
States calculate eligibility using Modified Adjusted Gross Income, which sounds complicated but basically means your tax return income with some adjustments. Wages, salary, tips, freelance income, unemployment benefits, and Social Security all count. What doesn't count? Things like child support in many states, student financial aid, and certain tax deductions.
The household size calculation works in your favor during pregnancy. You count yourself, your unborn baby (or babies if you're carrying twins or triplets), your spouse if you live together, and dependent children. A pregnant woman with one existing child equals a household of three for application purposes. That classification significantly raises your qualifying income ceiling.
Income Thresholds for Pregnancy Medicaid by State
| State | FPL Percentage | Monthly Income Cap (3-Person Household) | Additional Information |
| California | 213% | $4,600 | Available through Medi-Cal program |
| Texas | 198% | $4,270 | Program specifically for pregnant individuals |
| Florida | 191% | $4,120 | Coverage available despite no expansion |
| New York | 223% | $4,810 | Vision and dental included in benefits |
| Illinois | 213% | $4,600 | Full-year postpartum coverage guaranteed |
| Pennsylvania | 215% | $4,640 | Fast-track processing for urgent cases |
| Ohio | 200% | $4,320 | Immediate eligibility at participating clinics |
| Georgia | 220% | $4,750 | Apply through state Gateway system |
| North Carolina | 196% | $4,230 | Standard two-month postpartum period |
| Michigan | 195% | $4,210 | Connects to Healthy Michigan afterward |
| Virginia | 203% | $4,380 | Year-long postpartum extension started 2025 |
| Washington | 210% | $4,530 | Offered through Apple Health program |
| Arizona | 156% | $3,370 | Emergency delivery always covered |
| Massachusetts | 200% | $4,320 | Part of MassHealth Standard coverage |
| Tennessee | 250% | $5,400 | Among the nation's most generous limits |
You'll need to verify income with recent documentation. Gather your last four weeks of pay stubs if you're employed. Self-employed applicants need different paperwork—business bank statements, quarterly estimated tax payments, or a profit-and-loss statement for the current year work well. Tax returns from last year help but might not reflect your current situation if circumstances changed.
Income that bounces around seasonally? Case workers calculate based on what you reasonably expect to earn across the full year, then divide by 12 for a monthly figure. If you work retail and earn more during holidays, or you're a teacher without summer income, explain that pattern in your application.

Author: Derek Whitmore;
Source: blaverry.com
How to Apply for Pregnancy Medicaid
Apply the week you see that positive pregnancy test. Seriously—don't wait. You want coverage secured before calling an OB-GYN for your first appointment.
Multiple paths lead to the same destination. Your state Medicaid website offers online applications that process fastest, usually within two to three weeks. Healthcare.gov works too, though it redirects you to your state's system. Prefer in-person help? Visit your county Department of Social Services, a community health center, or a hospital with enrollment specialists on staff.
Many women don't realize hospitals employ people whose entire job involves helping with Medicaid applications. Schedule a prenatal visit at a hospital-affiliated clinic, mention you're uninsured, and ask to speak with their Medicaid enrollment counselor. They'll complete your application during that visit, often securing presumptive eligibility before you leave.
Online applications move fastest. Create an account on your state's benefits portal, answer questions about who lives in your home and what everyone earns, upload photos of your documents, and submit. You'll receive a confirmation number immediately—screenshot it or write it down. Processing typically wraps up within 15 to 30 business days, sometimes faster if your case is straightforward.
Paper applications remain an option, though they crawl along at a slower pace. Pick up forms at social services offices, complete them by hand, and mail or fax them in. Expect 30 to 45 days for processing. This route works fine if you're early in pregnancy and not yet scheduling appointments, but online is almost always better.
Presumptive eligibility deserves special mention. Participating health centers, hospitals, and community clinics can activate temporary Medicaid coverage during your visit, based on a quick income screening. This temporary coverage—usually lasting 60 days—buys time for your full application to process without leaving you uninsured.

Author: Derek Whitmore;
Source: blaverry.com
Required Documents and Information
Before starting your application, round up these items:
- Pregnancy confirmation (doctor's note, lab results from a positive test, or even just your attestation in some states)
- Government-issued photo ID (driver's license, state ID card, or passport)
- Social Security numbers for household members (if you have them)
- Proof you live in the state (utility bill from the past month, current lease, mortgage statement, or official mail with your address)
- Income verification (last month of pay stubs, most recent tax return, W-2 forms, or a letter from your employer on company letterhead)
- Bank statements covering the previous 30 days (required in some states, not others)
- Immigration paperwork (green cards, visas, naturalization certificates—if applicable)
Missing something? Apply anyway. Write a note in the application explaining which document you can't provide and why. Caseworkers can request missing pieces later. Many states accept your word about being pregnant until you visit a provider who can confirm it medically.
The old Medicaid asset tests—where owning a car or having savings disqualified you—don't apply to pregnancy coverage anymore. Your 401k balance and savings account won't derail your application. States focus exclusively on monthly income.
What to Do If Your Application Is Denied
Denial notices arrive by mail with a specific reason: income too high, missing paperwork, couldn't verify residency, or similar issues. You've got 90 days in most states to request an appeal—called a "fair hearing" in Medicaid terminology.
Don't ignore denials assuming the decision is final. Common calculation mistakes happen. Caseworkers sometimes forget to count your unborn child in household size, or they use gross income from your paycheck instead of net income with allowable deductions. These errors are fixable.
Request your hearing in writing immediately. Some states let you email or call, but written requests create documentation. While your appeal waits—hearings can take 30 to 60 days to schedule—ask whether your coverage continues during the process. Many states maintain benefits if you request the hearing quickly, usually within 10 days of the denial date.
If you genuinely earn too much for pregnancy Medicaid, explore two alternatives. First, CHIP programs in some states cover pregnant women at higher income levels than Medicaid. Second, losing Medicaid eligibility or being denied creates a Special Enrollment Period for Healthcare.gov plans. Those marketplace plans come with sliding-scale subsidies that might make coverage affordable—sometimes under $100 monthly.
What Pregnancy Medicaid Covers
Coverage goes way beyond just delivering your baby. You're getting comprehensive healthcare from your first prenatal visit through weeks after delivery.
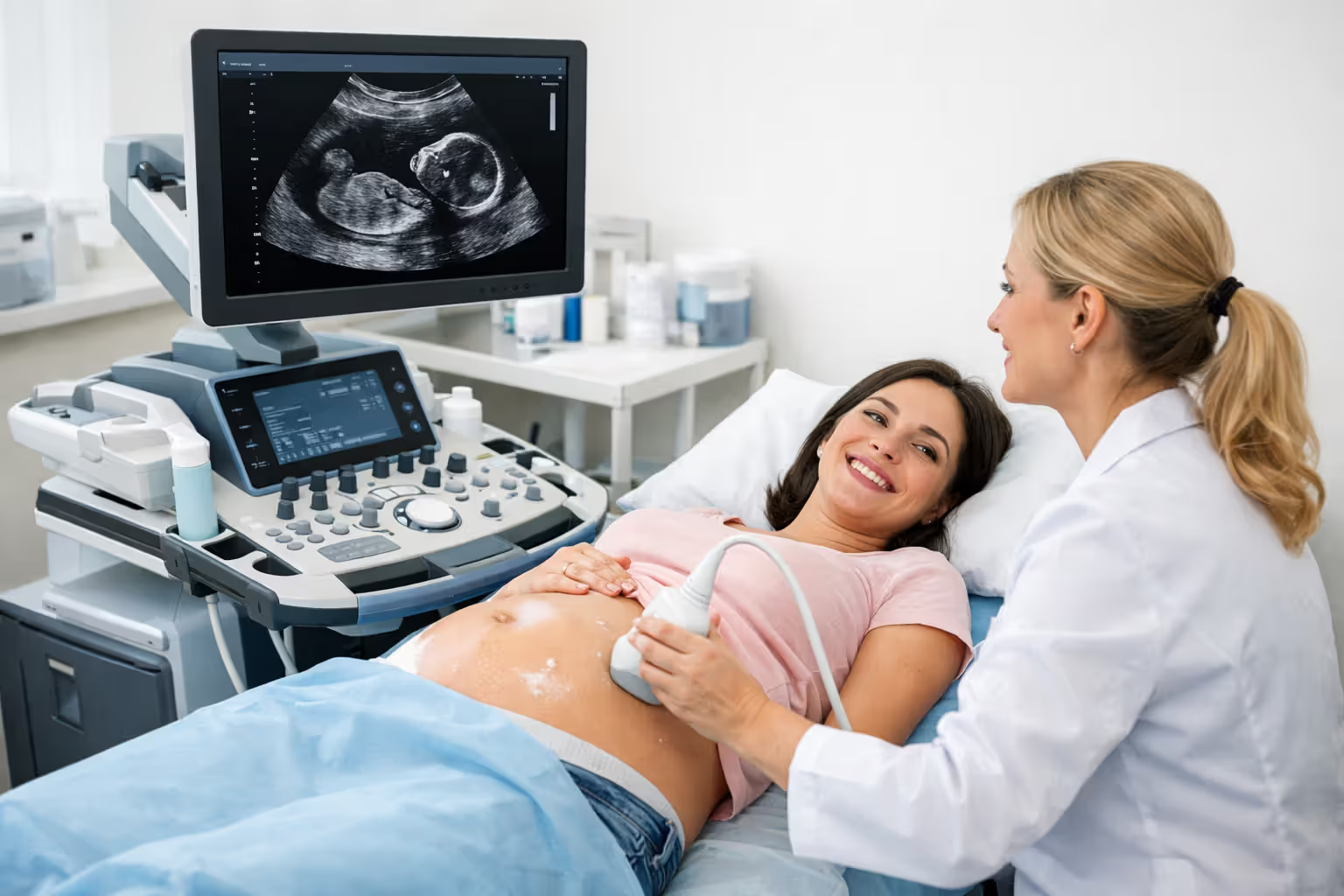
Prenatal care means all your regular checkups—typically once monthly until 28 weeks, then every two weeks until 36 weeks, then weekly until delivery. Every ultrasound is covered: the dating ultrasound around 8 weeks, the detailed anatomy scan at 20 weeks, and any additional imaging for complications. Blood work, urine tests, glucose screening for gestational diabetes, Group B strep testing—all covered without copays.
High-risk pregnancies receive extra monitoring at no charge. Weekly non-stress tests in your third trimester? Covered. Biophysical profiles to check amniotic fluid and fetal movement? Covered. Appointments with maternal-fetal medicine specialists? Covered. There's no tier system where certain specialists cost more.
Labor and delivery expenses—regardless of how your baby arrives—are fully covered. Hospital stay, obstetrician fees, anesthesiologist charges for your epidural, operating room costs for cesareans, any necessary interventions like forceps or vacuum assistance—none of it generates bills. If you end up hospitalized for a week due to complications like preeclampsia, that extended stay is covered too.
Postpartum care includes your six-week follow-up appointment plus any additional visits. Developed an infection after delivery? Covered. Hemorrhaging that requires readmission? Covered. Perineal tear that needs rechecking? Covered. The 38 states with 12-month postpartum extensions provide full Medicaid coverage—not just pregnancy-related care—for that entire first year.
Prescription medications related to pregnancy cost nothing out-of-pocket. Prenatal vitamins, nausea medication like Zofran, antibiotics for infections, insulin or metformin for gestational diabetes, blood pressure drugs for preeclampsia—all covered. Postpartum contraception is included too: pills, patches, IUDs, implants, even permanent sterilization if you choose it.
Dental coverage expanded significantly in recent years. Research linking gum disease to preterm birth convinced states that dental care during pregnancy makes financial sense. Most states now cover cleanings, X-rays, fillings, root canals, and extractions throughout pregnancy. That nagging tooth pain you've ignored? Get it treated while you're pregnant and covered.
Mental health services matter just as much as physical care. Depression screening at prenatal visits, counseling sessions with therapists or social workers, psychiatric medication management, and inpatient treatment if needed—all fall under pregnancy Medicaid benefits. Postpartum depression affects roughly 1 in 7 new mothers, and your coverage includes treatment for it.
Author: Derek Whitmore;
Source: blaverry.com
Extras you might not expect: nutritional counseling with a registered dietitian, especially valuable if you develop gestational diabetes. Lactation consultant visits, both in-hospital after delivery and outpatient appointments if breastfeeding challenges arise. Breast pumps—hospital-grade if medically necessary, standard pumps for all. Transportation to medical appointments through state-arranged rides if you lack reliable transport.
Pregnancy Medicaid Renewal and Postpartum Coverage
Traditional pregnancy Medicaid lasted through the end of the month containing your 60th day postpartum. Deliver on January 15th, and your coverage continued through March 31st (since the 60th day landed in March).
That timeline shifted dramatically starting in 2025. The American Rescue Plan let states extend postpartum Medicaid to 12 full months using federal matching funds. By 2026, 38 states adopted this option, fundamentally changing the postpartum landscape.
Check your specific state's policy because this matters enormously. States with year-long postpartum coverage require no action from you during that period. Your pregnancy Medicaid automatically rolls through your baby's first birthday without renewal paperwork.
For the remaining states using 60-day postpartum coverage, you'll need to reapply for regular Medicaid before that window closes. Your state should mail renewal paperwork 30 to 45 days before your coverage ends. Some states handle this automatically, reassessing whether you qualify for standard Medicaid based on current income and household composition. Other states expect you to submit a new application.
Here's where many new mothers hit obstacles: regular adult Medicaid has much stricter income limits than pregnancy coverage. In Medicaid expansion states, you might qualify for coverage up to 138% of poverty level. In non-expansion states, income limits for adults without disabilities can be absurdly low—sometimes 18% of poverty level, meaning a parent of two would need to earn under $300 monthly to qualify. Effectively, you could lose coverage entirely despite earning poverty-level wages.
Report income changes during pregnancy within 10 days of when they occur. Lose your job? Report it, because you might qualify for additional benefits like food assistance. Get a raise that pushes you slightly over the income limit? Report it anyway—most states won't terminate pregnancy Medicaid mid-pregnancy once you're enrolled, but they'll need to know for post-delivery planning.
Your baby automatically gets enrolled in Medicaid separately when born to a Medicaid-covered mother. The hospital handles this enrollment, typically before discharge. Your newborn receives their own Medicaid identification number and coverage that lasts at least 12 months, completely independent of your eligibility status. Even if you lose postpartum Medicaid due to income, your baby stays covered.
Planning for post-Medicaid coverage prevents gaps. Losing Medicaid qualifies as a Special Enrollment Period for marketplace insurance through Healthcare.gov. You've got 60 days from your coverage end date to enroll in a private plan without waiting for open enrollment. Browse plans before you lose coverage so you can enroll immediately when the time comes.
Common Mistakes When Applying for Pregnancy Medicaid
Waiting too long tops the list of avoidable errors. Women who postpone applying until their second trimester miss out on first-trimester care that identifies complications early. That dating ultrasound around 8 weeks establishes your due date accurately—important for everything from when to do certain tests to whether labor starts too early. Genetic screening happens between 10 and 13 weeks. Wait too long to apply, and you'll miss these windows even after approval comes through.
Submitting incomplete applications delays processing for weeks. Upload all required documents together in one submission rather than sending your pay stub today, your ID tomorrow, and your proof of residency next week. Each piecemeal submission restarts processing timelines in some states. Can't find a required document? Include a written explanation of why it's missing and when you'll provide it, rather than leaving that section blank.
Miscounting household members undermines your application. Your unborn baby counts as a household member, expanding your household size and raising your income limit. A pregnant woman living alone is applying as a household of two, not one. Pregnant with twins? That's a household of three just for you and your babies-to-be. This single mistake can mean the difference between qualifying at $3,200 monthly and qualifying at $4,100 monthly.

Author: Derek Whitmore;
Source: blaverry.com
Overestimating income happens surprisingly often with variable schedules. If your hours fluctuate week to week, don't report your highest-earning week as typical. Calculate an average: add up your last month of pay stubs and divide by the weeks worked. Seasonal workers should annualize their income: estimate total yearly earnings, divide by 12, and use that monthly figure.
Assuming you don't qualify stops too many eligible women from applying. The pregnancy income thresholds are dramatically more generous than other assistance programs. You might have been denied food stamps or regular Medicaid in the past, but pregnancy changes the calculation entirely. Teachers, nurses, retail managers, and small business owners enroll in pregnancy Medicaid every day. Apply regardless of assumptions.
Ignoring income change reporting requirements creates problems down the line. Lost your job during pregnancy? Report it within 10 days. Your income decreased, potentially qualifying you for emergency assistance. Hours got cut? Report it. Got a raise? Report that too. Some women avoid reporting positive changes, fearing they'll lose coverage, but failure to report can result in owing back payments or jeopardizing future applications.
Missing information request deadlines results in automatic application closures. Caseworkers mail requests for additional documents or clarification, always including a deadline—typically 10 to 14 days from the notice date. Life gets hectic, mail gets buried, and suddenly that deadline passed. Your application closes, requiring you to start from scratch. Set phone reminders when you receive these requests.
Confusing Medicaid with marketplace insurance frustrates many applicants. If you apply through Healthcare.gov and income screening shows you're Medicaid-eligible, the system transfers your application to your state Medicaid program. This redirect confuses people expecting to choose a commercial insurance plan. Understand that Medicaid eligibility blocks access to marketplace subsidies by design—you can't have both, and Medicaid provides more comprehensive coverage anyway.
The biggest misconception I encounter is pregnant women believing they earn too much to qualify. I've enrolled teachers, nurses, and small business owners who never imagined they'd be eligible. The pregnancy income limits are designed to be inclusive, and I encourage every pregnant woman to apply regardless of their assumptions about eligibility. The worst outcome is a denial, but the best outcome is comprehensive care for you and your baby at no cost
— Jennifer Martinez
Frequently Asked Questions About Pregnancy Medicaid
Pregnancy Medicaid serves millions of expectant mothers each year who would otherwise struggle to afford prenatal care, delivery, and postpartum recovery. The program's relatively generous income thresholds reflect understanding that healthy pregnancies require comprehensive medical support, and that early prenatal care prevents expensive complications later.
Understanding your state's income limits, gathering documentation before starting your application, and applying early in pregnancy gives you the best chance of securing coverage seamlessly. The expansion of postpartum coverage to 12 months in most states represents meaningful progress in reducing maternal mortality and morbidity, particularly from conditions that emerge weeks or months after delivery.
Your assumptions about eligibility might be wrong. Income limits reach much higher than most people expect, and the application process, while document-intensive, is navigable with help available at community health centers, hospitals, and through certified enrollment counselors who assist at no charge.
Pregnancy should be about preparing for your baby, not worrying about medical bills. Pregnancy Medicaid exists specifically to eliminate those financial barriers, ensuring your health and your baby's wellbeing come first.










