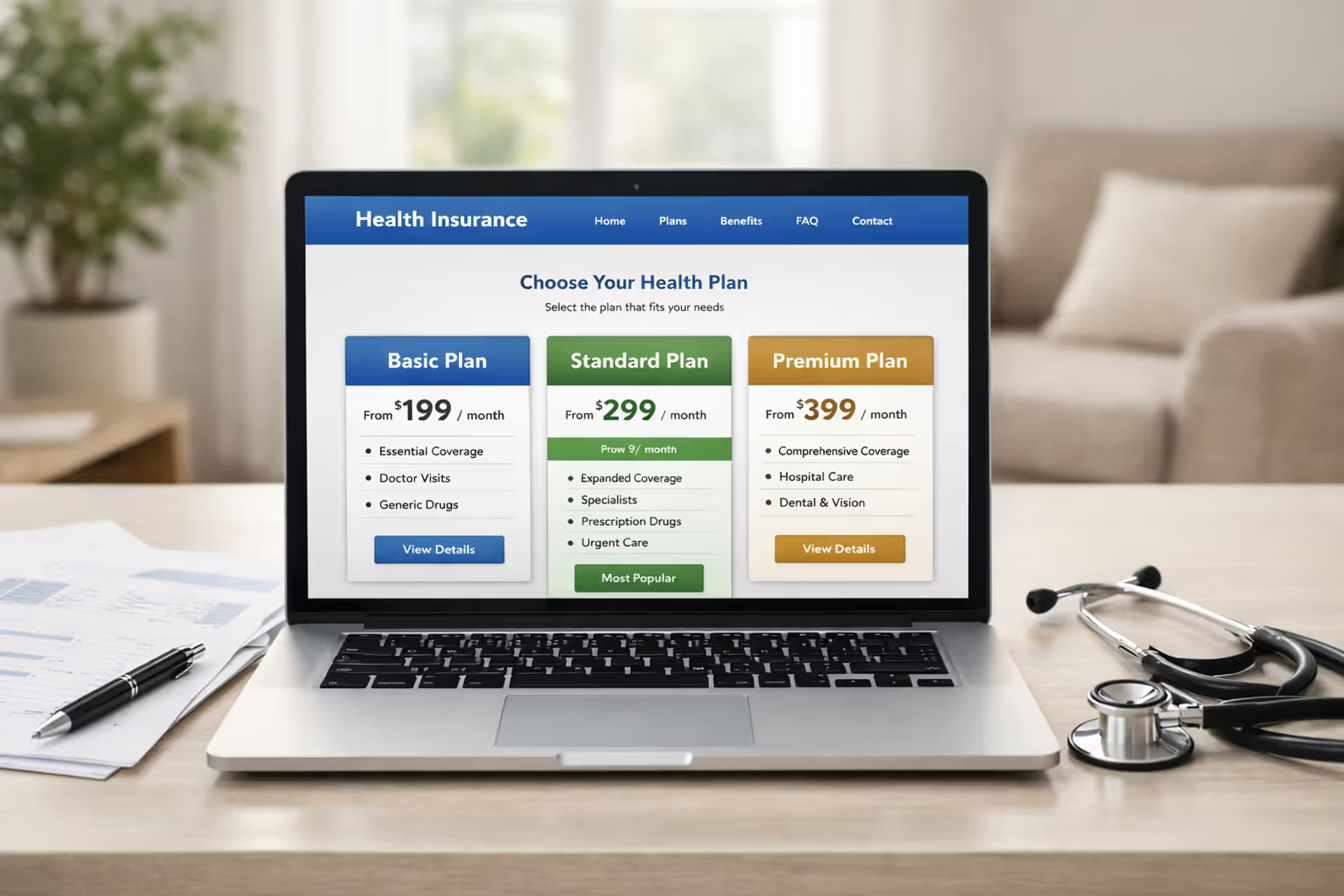
Laptop on a desk showing a health insurance marketplace website interface with plan comparison cards, stethoscope and documents nearby in a bright home office
What Is Marketplace Insurance and How Does It Work
Content
Choosing health coverage can feel overwhelming, especially when terms like "exchange" and "marketplace" get thrown around without clear explanation. If you've heard about marketplace insurance but aren't sure what it means for you, you're not alone. Millions of Americans use this system each year to find affordable health coverage, yet many eligible people never explore their options simply because the process seems confusing.
Marketplace insurance refers to health plans sold through government-run platforms created under the Affordable Care Act. These platforms—called Health Insurance Marketplaces or Exchanges—give individuals and families a centralized place to compare plans, check eligibility for financial help, and enroll in coverage. Understanding how this system works can save you thousands of dollars annually and ensure you get the protection you need.
Understanding Marketplace Insurance Basics
The Health Insurance Marketplace is an online shopping and enrollment service where you can compare private health insurance plans side-by-side. Think of it as a regulated platform where insurance companies offer their products under standardized rules. Every plan sold on the marketplace must cover ten essential health benefits, including emergency services, prescription drugs, maternity care, and mental health treatment.
Two types of marketplaces exist: the federal marketplace (HealthCare.gov) and state-based marketplaces. As of 2026, roughly half of U.S. states run their own exchanges with unique websites and branding—California uses Covered California, New York has NY State of Health, and so on. The remaining states use the federal platform or a hybrid model where the state handles certain functions while the federal government manages enrollment technology.
What is marketplace insurance in practical terms? It's private insurance with government oversight. The marketplace doesn't provide insurance itself; instead, it acts as a regulated storefront where private insurers compete for your business. The Affordable Care Act established these exchanges to solve a problem: before 2014, people without employer coverage often faced sky-high premiums, coverage denials for pre-existing conditions, or plans that didn't cover basic services. The marketplace standardized offerings and introduced subsidies to make coverage accessible.
The federal government sets annual open enrollment periods—typically November through mid-January—when anyone can sign up. Outside these windows, you need a qualifying life event like losing job-based coverage, getting married, having a baby, or moving to a new state.
Who Qualifies for Marketplace Health Insurance
Most U.S. citizens and lawfully present immigrants can purchase health insurance from the marketplace. You must live in the United States and not be incarcerated. Unlike Medicaid, there's no upper income limit for buying marketplace plans—a millionaire can purchase coverage if they want—but financial assistance is income-based.
Here's where it gets nuanced. If your employer offers health insurance that meets federal "affordability" and "minimum value" standards, you can still buy a marketplace plan, but you won't qualify for premium subsidies. In 2026, employer coverage is considered affordable if your share of the premium for self-only coverage doesn't exceed 9.02% of your household income. Many people discover their employer's family coverage costs far more than this threshold, yet they're still locked out of subsidies because the calculation only considers the employee-only premium—a frustrating quirk known as the "family glitch," which was partially addressed in recent regulations.
Citizenship and immigration status matter. U.S. citizens and nationals qualify immediately. Lawfully present immigrants—including green card holders, refugees, asylees, and those with certain visa types—are eligible. Undocumented immigrants cannot purchase marketplace plans, even at full price without subsidies, though some states offer separate programs using state funds.
Income levels determine subsidy eligibility. For 2026, premium tax credits are available to households earning between 100% and 400% of the federal poverty level, with enhanced subsidies extending beyond 400% for many families thanks to recent legislative changes. A single person earning roughly $15,060 to $60,240 would likely qualify for some assistance, though exact amounts vary by age, location, and household size.
Special enrollment periods open a 60-day window after qualifying events. Losing health coverage (including aging off a parent's plan at 26), getting married or divorced, having a baby, or moving to a new ZIP code all trigger eligibility. You'll need documentation—termination letters, birth certificates, marriage licenses—to prove your qualifying event.
Author: Ethan Bradford;
Source: blaverry.com
Types of Plans Available on the Insurance Marketplace
Insurance on the marketplace comes in standardized "metal tiers" that indicate how costs are split between you and the insurer. This system makes comparison shopping easier, though it confuses many first-time buyers who assume higher tiers always mean better coverage.
Bronze plans have the lowest monthly premiums but highest out-of-pocket costs when you need care. They typically cover 60% of healthcare expenses, leaving you responsible for 40%. Silver plans hit a 70/30 split. Gold plans cover 80%, and Platinum plans cover 90%. These percentages represent averages across a population—your actual split for any given service depends on whether you've met your deductible.
Catastrophic plans exist for people under 30 or those with hardship exemptions. These ultra-low-premium options cover three primary care visits and preventive services before the deductible, then kick in only after you've spent roughly $9,450 out-of-pocket in 2026. They protect against worst-case scenarios but offer little help with routine care.
Beyond metal tiers, you'll choose between plan structures like HMOs (Health Maintenance Organizations) and PPOs (Preferred Provider Organizations). HMOs typically cost less but require you to stay within a specific provider network and get referrals to see specialists. PPOs offer more flexibility—you can see out-of-network providers and skip referrals—but charge higher premiums and deductibles. Some marketplaces also offer EPOs (Exclusive Provider Organizations) and POS (Point of Service) plans, which blend features of both.
Every marketplace plan covers essential health benefits: ambulatory patient services, emergency services, hospitalization, maternity and newborn care, mental health and substance use disorder services, prescription drugs, rehabilitative services, laboratory services, preventive and wellness services, and pediatric services including dental and vision. Insurers can't cap annual or lifetime benefits, and they can't deny coverage or charge more based on health status.
Metal Tier Comparison Table
| Metal Tier | Avg. Monthly Premium | Typical Deductible | Out-of-Pocket Max | Insurance Pays | Best For |
| Bronze | $350–$450 | $6,000–$7,500 | $9,450 | ~60% | Healthy individuals who rarely need care and want catastrophic protection |
| Silver | $450–$600 | $3,500–$5,500 | $9,450 | ~70% | Most people; required for cost-sharing reductions if eligible |
| Gold | $550–$750 | $1,500–$3,000 | $9,450 | ~80% | Those with regular prescriptions or planned medical procedures |
| Platinum | $650–$900 | $0–$1,000 | $9,450 | ~90% | People with chronic conditions or high expected healthcare use |
Note: Premiums vary significantly by age, location, and tobacco use. Figures represent estimates for a 40-year-old non-smoker.
How to Enroll in Health Insurance From the Marketplace
Enrollment starts at HealthCare.gov for federal marketplace states or your state's exchange website. You'll create an account, then complete an application that asks about household size, income, current coverage, and citizenship status. The system estimates your subsidy eligibility in real-time, showing you the actual premium you'd pay after financial help.
Gather these documents before starting: Social Security numbers for everyone in your household, immigration documents if applicable, employer and income information (pay stubs, W-2s, or tax returns), and policy numbers for any current health insurance. If you're self-employed, you'll need profit and loss statements or a letter from your accountant estimating annual income.
The application takes 30 to 60 minutes for most people. You'll estimate your 2026 income—your best guess is fine, and you can update it later if circumstances change. The marketplace uses modified adjusted gross income (MAGI), which includes wages, self-employment income, Social Security benefits, investment income, and other taxable income, but excludes certain deductions.
After submitting your application, you'll see plans available in your area. You can filter by premium cost, deductible, provider network, and whether your doctors are in-network. Each plan listing shows the monthly premium after subsidies, deductible, out-of-pocket maximum, and a summary of benefits. Click into individual plans to see detailed coverage information, including prescription drug formularies and provider directories.
Once you select a plan, you'll pay your first month's premium directly to the insurance company—not through the marketplace. Coverage typically starts the first day of the following month if you enroll by the 15th. Enroll after the 15th, and coverage begins the month after that. During the final days of open enrollment, special rules may apply to ensure January 1 coverage.
Free help is available from navigators, certified application counselors, and insurance agents who specialize in marketplace plans. These professionals can walk you through the application, explain plan differences, and help you determine which tier makes financial sense. Find local assistance through the marketplace website or by calling the marketplace call center.

Author: Ethan Bradford;
Source: blaverry.com
Subsidies and Financial Assistance Options
Premium tax credits reduce your monthly insurance bill based on income and local coverage costs. The marketplace calculates these automatically when you apply. You can take the credit in advance—lowered premiums each month—or pay full price and claim the credit when filing taxes. Most people choose advance credits because paying $150 monthly beats paying $600 and waiting months for a $5,400 tax refund.
The credit amount ensures you don't pay more than a set percentage of income for the second-lowest-cost Silver plan in your area. In 2026, someone earning 150% of the poverty level pays roughly 3% to 4% of income for this benchmark plan, while someone at 300% pays around 8% to 9%. If the actual premium exceeds your capped contribution, the government covers the difference.
Cost-sharing reductions (CSRs) lower your deductibles, copays, and out-of-pocket maximums, but they're only available with Silver plans and only if your income falls between 100% and 250% of poverty level. These reductions are substantial—a Silver plan with CSRs might have a $500 deductible instead of $5,000. You must actively choose a Silver plan to get this benefit; Bronze, Gold, and Platinum plans don't qualify.
Income changes affect subsidy amounts. Got a raise? Lost a job? Your tax credit should be adjusted. Log into your marketplace account and report changes within 30 days. If you don't update and receive more subsidy than you're entitled to, you'll owe the difference at tax time. Conversely, if your income drops and you don't report it, you're leaving money on the table.
Advanced premium tax credits create a reconciliation process on your tax return. Form 8962 compares the subsidy you received to what you actually qualified for based on final annual income. If you received too much, you repay the excess (with caps based on income). If you received too little, you get the remainder as a tax refund.
Marketplace Insurance vs. Other Coverage Options
Employer-sponsored insurance remains the most common coverage source for Americans under 65. If your job offers affordable, comprehensive coverage, it's often the better deal—employer plans typically have lower premiums because companies pay part of the cost, and provider networks are often broader. However, marketplace plans with subsidies can beat employer coverage for lower-income workers, especially if the employer's plan has high deductibles or limited networks.
Medicaid covers low-income individuals and families at little or no cost. In the 39 states that expanded Medicaid under the ACA, adults earning up to 138% of poverty level qualify. In non-expansion states, eligibility is far more restrictive—often limited to pregnant women, children, disabled individuals, and extremely low-income parents. If you qualify for Medicaid, you can't receive marketplace subsidies; Medicaid is always the first option.
Medicare serves people 65 and older and certain younger individuals with disabilities. You can't have both Medicare and marketplace coverage with subsidies. Once Medicare-eligible, you should enroll in Medicare Parts A and B, then decide whether to add Part D (prescription drugs) and a Medigap or Medicare Advantage plan.
Private insurance purchased outside the marketplace—directly from insurers or through brokers—offers identical coverage to marketplace plans in many cases. The same insurers sell the same plans in both places. The key difference: you can't receive subsidies for off-marketplace plans. If your income is too high for subsidies or you prefer working with a specific broker, buying outside the marketplace is perfectly fine. Plans must still meet ACA standards, including coverage of pre-existing conditions and essential health benefits.
Short-term health plans and health-sharing ministries are alternatives some people consider, but they're not comprehensive coverage. Short-term plans can deny coverage for pre-existing conditions, exclude entire categories of care, and impose lifetime limits. They're cheaper but riskier—fine as a brief stopgap, problematic as long-term coverage.
Expert Perspective:
Many people choose marketplace plans based solely on the monthly premium, which is a mistake.A Bronze plan with a $300 premium might seem like a great deal until you face a $7,000 deductible for a single emergency room visit. Understanding your expected healthcare use—regular prescriptions, planned surgeries, chronic condition management—is essential to choosing the right metal tier. For many families, a mid-tier Silver or Gold plan offers better financial protection, especially when cost-sharing reductions are available
— Jennifer Tolbert
Common Mistakes When Choosing Insurance on the Marketplace
Focusing exclusively on premium costs is the most frequent error. A Bronze plan saves you $100 monthly compared to Silver, but if you need regular care, you'll spend thousands more in deductibles and copays. Run the math: multiply your monthly premium by 12, then add estimated out-of-pocket costs for your typical healthcare use. The plan with the lowest total annual cost—premium plus expected expenses—is your best value.
Missing enrollment deadlines locks you out of coverage until the next open enrollment unless you have a qualifying life event. Mark your calendar for the annual open enrollment period, which typically runs from November 1 to mid-January. If you miss the deadline and don't qualify for special enrollment, you'll face a coverage gap and potential tax penalties in states that still enforce individual mandates.
Ignoring provider networks causes headaches. That cheap HMO looks great until you discover none of your doctors participate. Before enrolling, download the plan's provider directory and verify your doctors, specialists, and preferred hospitals are in-network. Call the providers' offices directly—online directories are sometimes outdated—and confirm they're accepting new patients with that specific plan.

Author: Ethan Bradford;
Source: blaverry.com
Failing to report income changes costs money. Got a new job with higher pay? Report it within 30 days to avoid owing thousands in excess subsidies at tax time. Income dropped? Update immediately to increase your monthly subsidy. The marketplace makes updates easy through your online account.
Forgetting to renew coverage is surprisingly common. The marketplace will auto-renew your plan if you don't actively choose a new one, but your subsidy amount will be based on outdated income information, and your current plan's price may have increased significantly. Log in during open enrollment each year, review available plans, update your income projection, and actively select the best option for the coming year.
Overlooking cost-sharing reductions leaves money on the table for eligible households. If your income qualifies you for CSRs, choosing a Bronze or Gold plan means forfeiting this benefit. Silver plans unlock the enhanced cost-sharing that dramatically lowers your deductibles and copays—often making Silver with CSRs a better deal than Gold without them.
Frequently Asked Questions
Navigating the Health Insurance Marketplace doesn't require expertise in healthcare policy or insurance jargon—it requires understanding your own needs, honestly estimating your income, and comparing plans based on total costs rather than just monthly premiums. The standardized metal tier system makes comparison shopping straightforward once you grasp that Bronze, Silver, Gold, and Platinum represent different cost-sharing arrangements, not different levels of medical quality.
For the roughly 20 million Americans who get coverage through marketplace plans in 2026, this system provides access to comprehensive insurance that would otherwise be unaffordable or unavailable. The subsidy structure means that even middle-income families can find plans that cost less than 10% of their income, and cost-sharing reductions give lower-income households access to plans with deductibles they can actually afford to meet.
Start by gathering your documents, estimating your annual income accurately, and setting aside time to compare at least three plans in different metal tiers. Consider your expected healthcare needs—regular prescriptions, planned procedures, chronic conditions—and calculate total annual costs including premiums and anticipated out-of-pocket expenses. Check provider networks carefully, and don't hesitate to use free assistance from navigators or certified counselors who can explain your options without pressure.
The marketplace isn't perfect. Plan options vary dramatically by location, and some rural areas have limited insurer participation. But for individuals and families without access to employer coverage, it remains the best path to comprehensive, affordable health insurance. Understanding how marketplace insurance works transforms it from a confusing bureaucratic maze into a practical tool for protecting your health and finances.










