
Young couple sitting at kitchen table reviewing health insurance documents on laptop
Can I Add My Boyfriend to My Health Insurance
Content
You've probably heard coworkers mention adding their spouse to their company health plan. Straightforward, right? But what about adding your boyfriend—someone you're committed to but haven't married? Here's where things get interesting.
The reality? It's definitely possible in many cases, though it's rarely as simple as filling out a form. Your employer might say yes. They might say no. Or they might say "yes, but only if you jump through these specific hoops first."
What makes adding a boyfriend different from adding a spouse? Two things: documentation requirements are significantly more involved, and the IRS treats the premium contributions your employer makes completely differently—in a way that'll show up on your tax bill.
When You Can Add a Boyfriend to Your Health Insurance
So when does this actually work? You need two things to align: your employer has to allow it, and you typically need to meet certain relationship criteria your company sets.
Domestic Partner Requirements by State
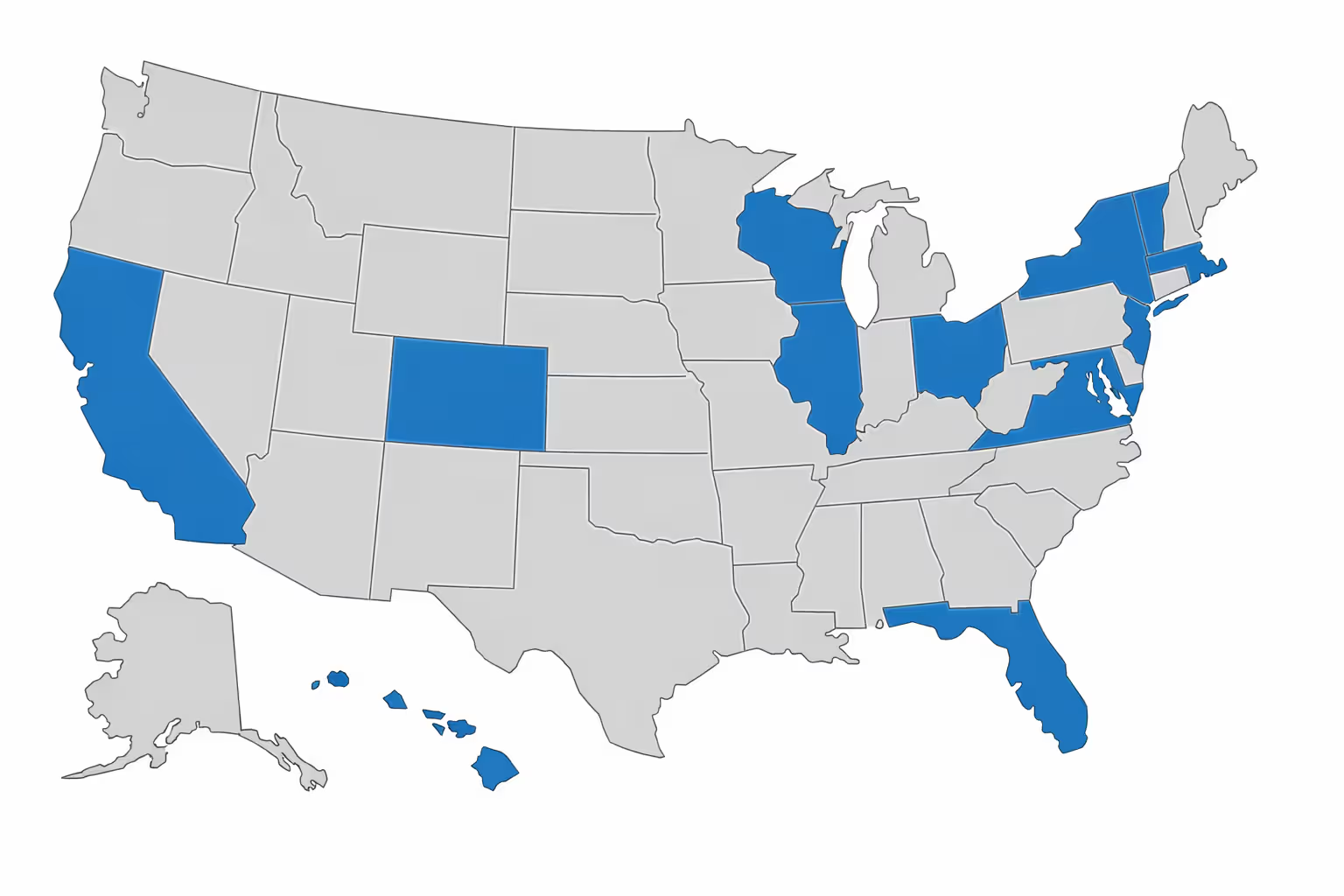
Right now, fifteen states plus Washington D.C. run official registries where unmarried couples can formally register their partnerships. We're talking about California, Oregon, Washington, Nevada, Colorado, Maine, New Jersey, Rhode Island, Vermont, Hawaii, Illinois, Wisconsin, Connecticut, and D.C.
What does getting registered usually involve? Here's what most registries ask:
- You're both at least 18
- Neither of you is currently married
- You live together and consider it a committed, long-term relationship
- Your finances are intertwined—think shared checking accounts, both names on the lease, maybe a car loan together
- You're not closely related (no situations where marriage would be illegal due to family connection)
Now, not every state runs a formal registry. In those places, many employers accept what's called a domestic partnership affidavit instead. Basically, you're swearing under oath that your relationship meets their criteria. But here's the catch—you can't just sign the form and call it done. You'll need backup evidence: maybe six months of bank statements from your joint account, utility bills addressed to both of you, or perhaps a car insurance policy listing you both.
Here's something people often miss: certain cities run their own registries even when their state doesn't. Take New York City. New York State doesn't maintain a statewide registry, but NYC does—and plenty of insurance companies respect that city registration.
Author: Ethan Bradford;
Source: blaverry.com
Employer Plan Rules and Eligibility
Federal law doesn't force any employer to cover domestic partners. Zero requirement. Each company decides for themselves.
You'll find this benefit more commonly at larger corporations, particularly tech companies and companies competing hard for talent. Smaller businesses? Less common, though it's not unheard of.
Where do you find out if your company allows it? Check your benefits guide or employee handbook. Look specifically at the section describing "eligible dependents." If it only mentions spouse and children, you're probably out of luck unless you establish a formally recognized partnership first.
Companies that self-fund their health plans—meaning they pay medical claims directly instead of buying traditional insurance—have more wiggle room to write their own eligibility rules. Companies buying traditional insurance policies need to work within whatever rules their state insurance regulators set.
One requirement that pops up constantly: proof that you actually live together, usually for a minimum period. Six months is common. A full year isn't unusual. Your company wants evidence you've established a genuine shared household, not just moved in together last month specifically to get insurance coverage.
How Domestic Partnership Differs from Marriage for Coverage
Getting married creates an instant special enrollment window. You've got 30 to 60 days after your wedding to add your new spouse, regardless of when open enrollment happens. Super convenient.
Domestic partnerships? Way less standardized. Some employers treat partnership registration exactly like marriage—you get that same special enrollment window. Others make you wait until open enrollment rolls around again. You really need to ask HR how your specific company handles it.
But here's the big financial difference that catches people off guard: taxes.
When your employer pays part of your spouse's premium—let's say they kick in $400 a month—the IRS doesn't count that as income to you. It's tax-free. Nice benefit.
For a domestic partner? Unless your boyfriend qualifies as your tax dependent (and we'll get to why that's unlikely), the IRS says that $400 monthly employer contribution is taxable income. It gets added to your W-2 as "imputed income," and you pay regular income tax plus payroll tax on it.
For your boyfriend to qualify as a tax dependent, three things need to be true:
- He lives with you the entire year
- His income is below $5,300 for the year (the 2026 threshold)
- You provide more than half his financial support
Most adults with jobs fail that income test immediately. If your boyfriend works full-time, he almost certainly makes more than $5,300 annually.
So what does this tax hit actually cost? Let's say your employer contributes $400 monthly toward his coverage. That's $4,800 yearly. If you're in the 24% federal bracket and you add FICA taxes, you're looking at roughly $1,500 in additional tax liability. That's $125 a month in extra taxes you wouldn't pay if you were married.
Documentation demands are also totally different. Marriage certificate? One document, done. Domestic partnership? You're typically submitting:
- The completed domestic partnership affidavit your company provides
- Lease or mortgage showing both your names (or multiple utility bills if only one name is on the housing contract)
- Joint bank account statements going back several months
- Maybe beneficiary designation forms where you've named each other
- Your state or city partnership certificate if you registered officially
- Sometimes notarized sworn statements
Why so much paperwork? Insurance fraud. Companies worry about people claiming roommates or friends as partners to get them coverage, so they verify carefully.
Alternative Ways to Get Your Boyfriend Health Coverage
Maybe your employer doesn't offer partner benefits. Or perhaps you don't meet the qualification requirements. What then?
Marketplace Plans and Subsidies

Author: Ethan Bradford;
Source: blaverry.com
He can always buy his own coverage through HealthCare.gov (or your state's exchange if they run their own). Open enrollment runs November 1 through mid-January in most places, though some states extend it longer.
Premium subsidies make marketplace plans genuinely affordable for many people. For 2026, individuals earning between roughly $15,060 and $60,240 qualify for tax credits that reduce monthly premiums—sometimes dramatically.
Real example: someone making $35,000 might pay $175 monthly for a Silver plan after subsidies, compared to $450 without assistance. That's a $275 monthly discount.
Cost-sharing reductions sweeten the deal further for people earning under approximately $37,650. These enhanced Silver plans lower your deductible and copays, sometimes offering better value than employer coverage.
Here's an interesting angle: because you're not married, you file taxes separately and each person's subsidy eligibility depends only on their individual income. If you were married, your combined household income would determine qualification. For some couples, staying unmarried actually results in better financial assistance.
COBRA and Short-Term Options
Lost his job recently? COBRA extends his old employer coverage for 18 months, though he pays the full premium plus a 2% admin fee. Expensive, but it makes sense when he's in the middle of treatment or needs to keep his current doctors.
Short-term plans fill temporary gaps—usually three to twelve months. They cost less because they cover less. Pre-existing conditions? Not covered. Preventive care? Usually excluded. They work for healthy people between jobs, not as a permanent solution.
Warning: in California, Massachusetts, New Jersey, Rhode Island, Vermont, and D.C., short-term plans don't satisfy state individual mandate requirements. You could owe a tax penalty at tax time.
Medicaid Eligibility
In the 41 states that expanded Medicaid, adults earning up to roughly $20,780 (138% of poverty level for 2026) qualify. Medicaid provides comprehensive coverage with little to no premiums and minimal cost-sharing.
Because you're unmarried, Medicaid looks only at his income, not yours. Even if you make six figures, he might still qualify based on what he personally earns.
There's no waiting period or open enrollment restriction for Medicaid. Eligible now? Apply now. Coverage typically starts the month after approval.
Common Mistakes When Adding a Partner to Health Insurance
People trip over several common obstacles when enrolling domestic partners.
Misunderstanding enrollment timing. Marriage triggers a special enrollment period—you get those 30 to 60 days to add coverage whenever the wedding happens. Many people assume registering a domestic partnership works the same way. Sometimes it does. Sometimes it absolutely doesn't, and you're stuck waiting until your company's annual enrollment period. Imagine registering your partnership in March, then discovering you can't add insurance coverage until the following January. Check with HR before you assume anything.
Submitting inadequate documentation. One utility bill and a recently-signed lease rarely cut it. Employers want evidence of an established relationship, which means multiple documents spanning several months. That joint checking account you opened two weeks ago? Probably won't satisfy the requirement. Start building your paper trail at least six months before you plan to enroll.
Underestimating the tax impact. That $350 monthly employer contribution sounds great until you realize it adds $4,200 to your taxable income. At a 25% effective tax rate, you're paying an extra $1,050 in taxes annually—$87.50 every month. Some couples discover that marketplace coverage with subsidies actually costs less than employer coverage after accounting for these taxes. Calculate the real after-tax cost before deciding.
Failing to notify HR after breakups. Divorce creates legal documentation automatically. Breaking up? Not so much. You must tell your employer within 30 days when a domestic partnership ends. Skip this step and you're covering someone who's no longer eligible—potential fraud territory, plus tax complications you don't want.
Assuming your new job works like your old one. Your previous employer might have offered partner benefits with minimal fuss. Your new employer might require state registration plus six months of cohabitation documentation. Every company writes their own rules. Never assume policies transfer.
Forgetting about registry renewals. Some states require periodic renewal of domestic partnerships. California partnerships established before 2012 needed renewal (newer ones don't). Let your registration lapse without renewing, and your boyfriend could lose coverage mid-year with no warning.

Author: Ethan Bradford;
Source: blaverry.com
Cost Differences: Adding a Domestic Partner vs Spouse
The financial comparison helps clarify your best option.
| Factor | Adding Spouse | Adding Domestic Partner |
| Monthly premium increase | Typically $200–$600 based on plan | Usually $200–$600 (same base amount) |
| How much employer pays | Often covers 50–75% of dependent cost | Same percentage, but triggers tax consequences |
| IRS treatment | Employer portion isn't taxable | Employer portion added to your taxable income unless partner meets dependency tests |
| Documents needed | Just marriage certificate | Affidavit, proof you live together, evidence of financial interdependence, possibly state certificate |
| When you can enroll | Within 30–60 days of wedding, any time of year | Sometimes immediate, sometimes only during open enrollment—company dependent |
| Tax bill impact | No change | Typically $1,000–$2,000 extra yearly |
That tax difference matters more than most people realize initially. With a $350 monthly employer contribution ($4,200 yearly), you're in the 24% bracket, and FICA adds another 7.65%, you'll pay roughly $1,330 extra in taxes. Effectively, that's $110 monthly on top of whatever employee premium portion you already pay.
Sometimes marketplace coverage with subsidies actually costs less than adding a partner to employer coverage once you factor in imputed income taxes. Worth calculating both scenarios.
I see couples caught off guard by the W-2 impact constantly. They think domestic partner coverage costs the same as spousal coverage because the premium looks identical. Then tax time arrives and they're confused about the extra income reported. The coverage itself might cost the same from a premium standpoint, but that tax treatment fundamentally changes the financial equation. I tell everyone—calculate your actual after-tax expense before enrolling a partner
— Rennifer Morrison
Frequently Asked Questions About Adding a Boyfriend to Health Insurance
Can you add your boyfriend to your insurance? Often yes, assuming your employer permits domestic partner enrollment and you meet their relationship requirements. Expect more paperwork than adding a spouse would require, and prepare for the tax hit from imputed income on employer contributions.
Before you enroll him, crunch the actual numbers—premium cost plus tax impact—against what marketplace coverage with subsidies would run. Plenty of couples discover separate policies deliver better value, especially when income levels trigger substantial premium tax credits and cost-sharing reductions.
If domestic partner coverage makes financial sense for your situation, start documentation early. Open that joint checking account. Get both names on the lease or utility bills. Register your partnership if your state or city offers it. These things take time, and you want everything ready when your enrollment opportunity opens.
Domestic partner benefits have become more widespread over the past decade, but marriage still offers simpler enrollment and better tax treatment. Understanding your plan's specific requirements and calculating the true costs helps you choose what works best for both of you.










