
Young adult reviewing health insurance documents at a desk with a laptop and insurance card in a modern apartment
How Long Can You Be on Your Parents Health Insurance
Content
Understanding when your eligibility for parental health insurance coverage ends is critical for avoiding gaps in medical care. The Affordable Care Act established clear rules about dependent coverage, but confusion still surrounds the details, exceptions, and what happens when you age out of your parents' plan.
Age Limits and Basic Eligibility Rules
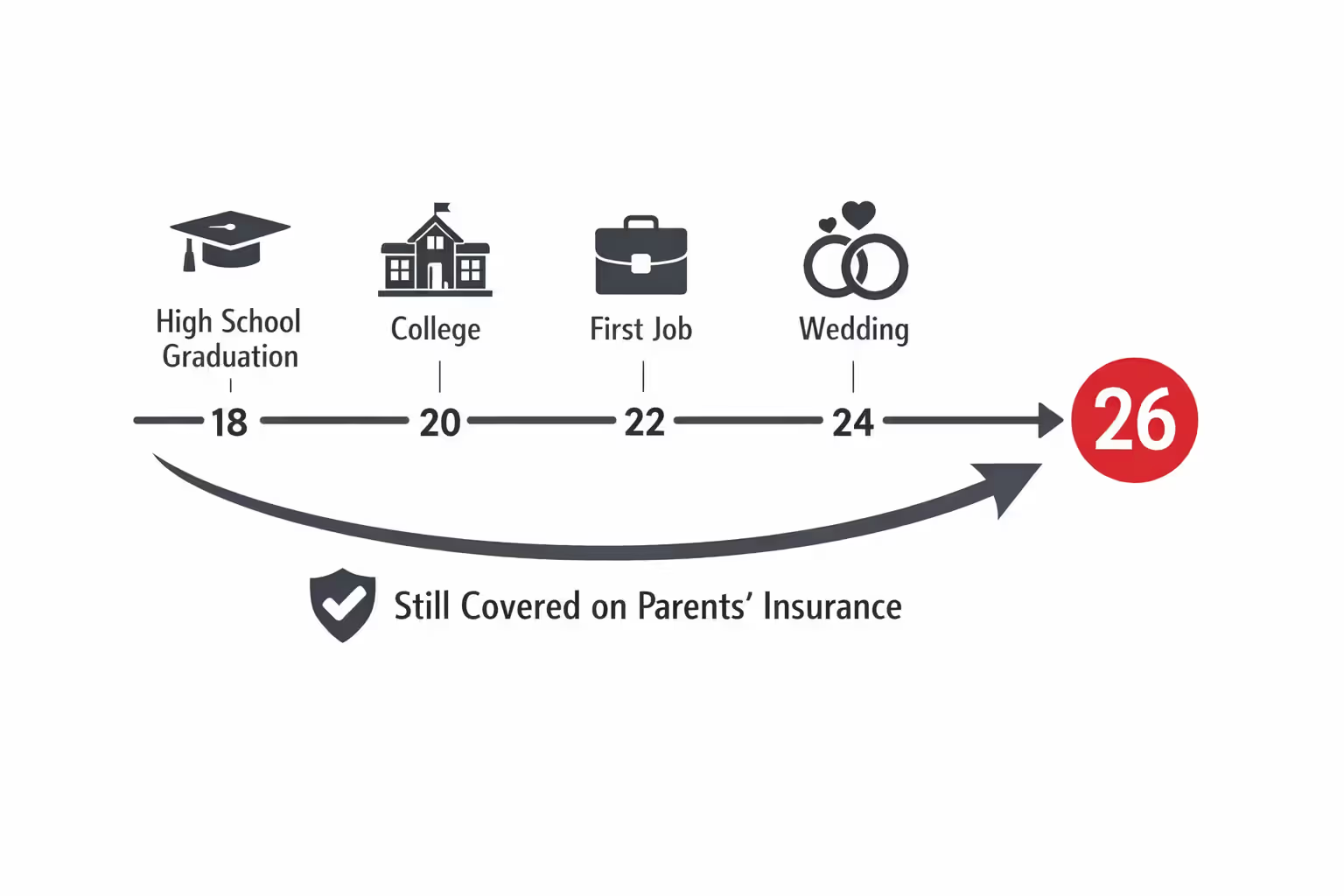
Federal law allows young adults to remain on their parents' health insurance until they turn 26 years old. This cutoff applies regardless of several factors that many people mistakenly believe affect eligibility.
Your coverage typically ends on your 26th birthday, though some plans extend through the end of the month or calendar year in which you turn 26. The specific termination date depends on your parent's plan language and state regulations.
Contrary to popular belief, getting married does not disqualify you from staying on your parents' insurance. You can be married with your own household and still maintain coverage under your parent's plan until age 26. Similarly, having a job—even one that offers health benefits—doesn't automatically remove you from eligibility. You can decline your employer's coverage and stay on your parent's plan if that arrangement works better financially.
Living arrangements don't matter either. You can live in a different state, attend college across the country, or maintain a completely independent household while remaining covered. Tax dependency status is also irrelevant; your parents don't need to claim you as a dependent on their tax returns for you to qualify for their health insurance.
The one universal rule: once you turn 26, your eligibility ends. No employment status, student status, or disability (with limited exceptions) changes this federal age limit under standard ACA provisions.
Author: Derek Whitmore;
Source: blaverry.com
How the Affordable Care Act Changed Dependent Coverage
Before 2010, health insurance companies imposed numerous restrictions on dependent coverage. Many plans terminated coverage when children turned 19, or 23 if they remained full-time students. Getting married, moving out, or becoming financially independent often triggered immediate loss of coverage.
Insurance companies could also refuse to cover young adults who had access to employer-sponsored insurance, even if that coverage was unaffordable or inadequate. This patchwork system left millions of young adults uninsured during a critical life transition period.
The Affordable Care Act, which took effect in September 2010, standardized dependent coverage rules nationwide. The law required all health plans that offer dependent coverage to allow children to stay on their parents' plans until age 26. This provision applied to both individual and employer-sponsored group plans.
This change represented a significant shift in how families could manage healthcare coverage. Young adults graduating college, starting careers, or pursuing entrepreneurial ventures gained flexibility to maintain continuous coverage during uncertain periods. The extended coverage window acknowledged that the path from adolescence to full financial independence had lengthened compared to previous generations.
The ACA provision applies to all job-based plans and individual market plans that cover dependents. Grandfathered plans (those existing before March 23, 2010) had to comply with the under-26 rule for plan years beginning on or after September 23, 2010, though they received some limited exceptions regarding children with access to employer coverage until 2014.
Special Circumstances That Affect Coverage Duration
While federal law sets age 26 as the standard cutoff, certain situations create exceptions or extensions to this rule.
Military Service and TRICARE
Young adults who serve in the military transition to TRICARE coverage, the health program for uniformed service members. Upon enlisting, they typically leave their parents' civilian health insurance and receive military healthcare benefits.
After completing military service, veterans under 26 may rejoin their parents' health insurance plan. This re-enrollment qualifies as a special enrollment event, allowing them to get back on the plan outside normal enrollment periods. The veteran must request enrollment within 60 days of losing TRICARE eligibility.
State-Specific Extensions Beyond Age 26
Several states have enacted laws extending dependent coverage beyond the federal age-26 limit. These state mandates apply only to fully insured plans regulated by state insurance departments—not to self-funded employer plans governed by federal ERISA law.
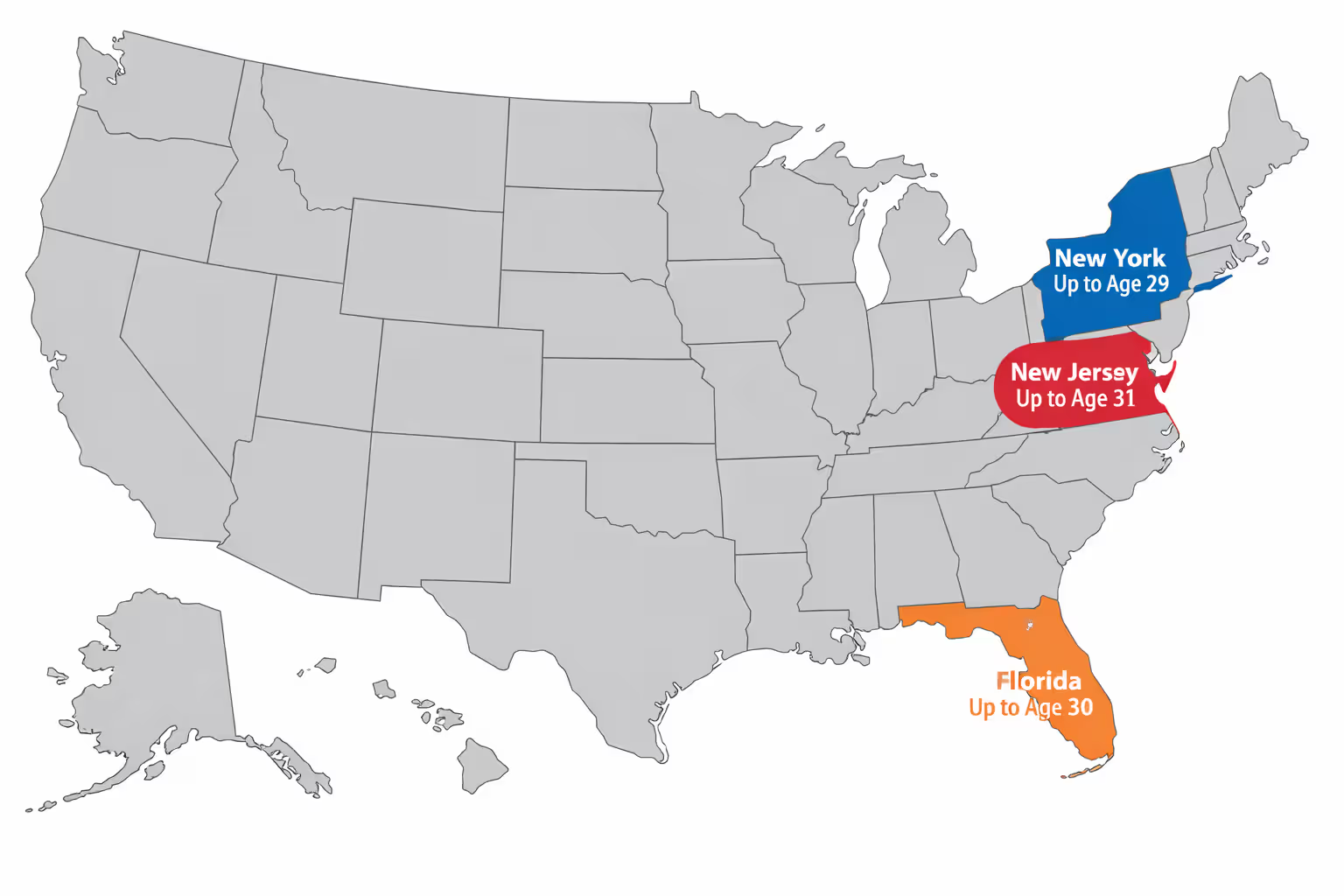
New York allows dependent coverage up to age 30 for unmarried dependents. Florida extends coverage to age 30 for unmarried dependents who lack access to employer coverage. New Jersey permits coverage until age 31 under certain circumstances.
These extensions typically require the young adult to meet specific criteria: residing in the state, lacking access to employer coverage, or remaining unmarried. The requirements vary significantly by state, and not all plans sold in these states must comply if they're self-funded employer plans.
Disability Status
Author: Derek Whitmore;
Source: blaverry.com
Young adults with disabilities that began before age 26 may qualify for extended dependent coverage beyond the standard age limit. This exception doesn't stem from the ACA but from plan-specific provisions and state laws that existed previously.
Plans that offer this extension require medical documentation proving the disability prevents the dependent from self-sustaining employment. The dependent must also rely on the parent for financial support. Insurers periodically review these cases to verify continued eligibility.
Parents should review their specific plan documents to understand whether disability extensions apply and what documentation requirements exist.
Comparing Parent Plan Coverage to Other Insurance Options
Staying on your parents' health insurance isn't always the best choice financially or practically. Understanding alternatives helps you make informed decisions.
| Coverage Type | Age Eligibility | Average Monthly Cost (2026) | When It Makes Sense |
| Parent's Plan | Under 26 | $0–$200 added to parent's premium | Parents have strong employer coverage; you're healthy; lower cost than alternatives |
| Employer Plan | Any age (if employed) | $150–$400 employee contribution | Your employer subsidizes premiums significantly; plan quality exceeds parent's plan; need employer HSA |
| Marketplace/ACA Plan | Any age | $200–$600 (before subsidies) | Income qualifies you for subsidies; you're self-employed; parents don't have coverage |
| Medicaid | Any age (income-based) | $0 | Income below state threshold (varies by state expansion status) |
| COBRA | After losing other coverage | $600–$800 (full premium plus 2%) | Short-term bridge (expensive); need to maintain same coverage temporarily |
Many young adults automatically assume their parents' plan is cheapest, but that's not always true. If your employer covers 80% of premium costs, your out-of-pocket expense might be lower than the amount your parents pay to add you to their plan.
Compare deductibles, copays, and provider networks too. Your parent's plan might have a high deductible that doesn't work well if you have regular medical needs. An employer plan with a lower deductible could save money despite higher premiums if you frequently visit doctors or take prescription medications.
Marketplace plans deserve consideration if your income qualifies you for premium tax credits. A 24-year-old earning $35,000 annually might pay just $100 monthly for a Silver plan after subsidies—potentially less than being added to a parent's employer plan.
What Happens When You Turn 26
Losing coverage at age 26 triggers a special enrollment period, giving you 60 days before and after your birthday to enroll in alternative coverage without waiting for annual open enrollment.
Most plans terminate coverage on your 26th birthday itself, though some extend through the end of that month. A few continue until the end of the calendar year or the plan year in which you turn 26. Check your parent's plan documents at least 90 days before your birthday to know the exact termination date.
Missing the special enrollment window creates serious problems. Without enrolling during those 60 days, you'll wait until the next annual open enrollment period (typically November through mid-January for coverage starting January 1). That could mean months without insurance.
COBRA coverage offers a backup option, allowing you to continue your parents' plan for up to 36 months by paying the full premium plus a 2% administrative fee. For most people, COBRA costs $600 to $800 monthly—significantly more than marketplace or employer alternatives. It makes sense only if you're mid-treatment for a serious condition and need to maintain the same doctors and coverage temporarily.
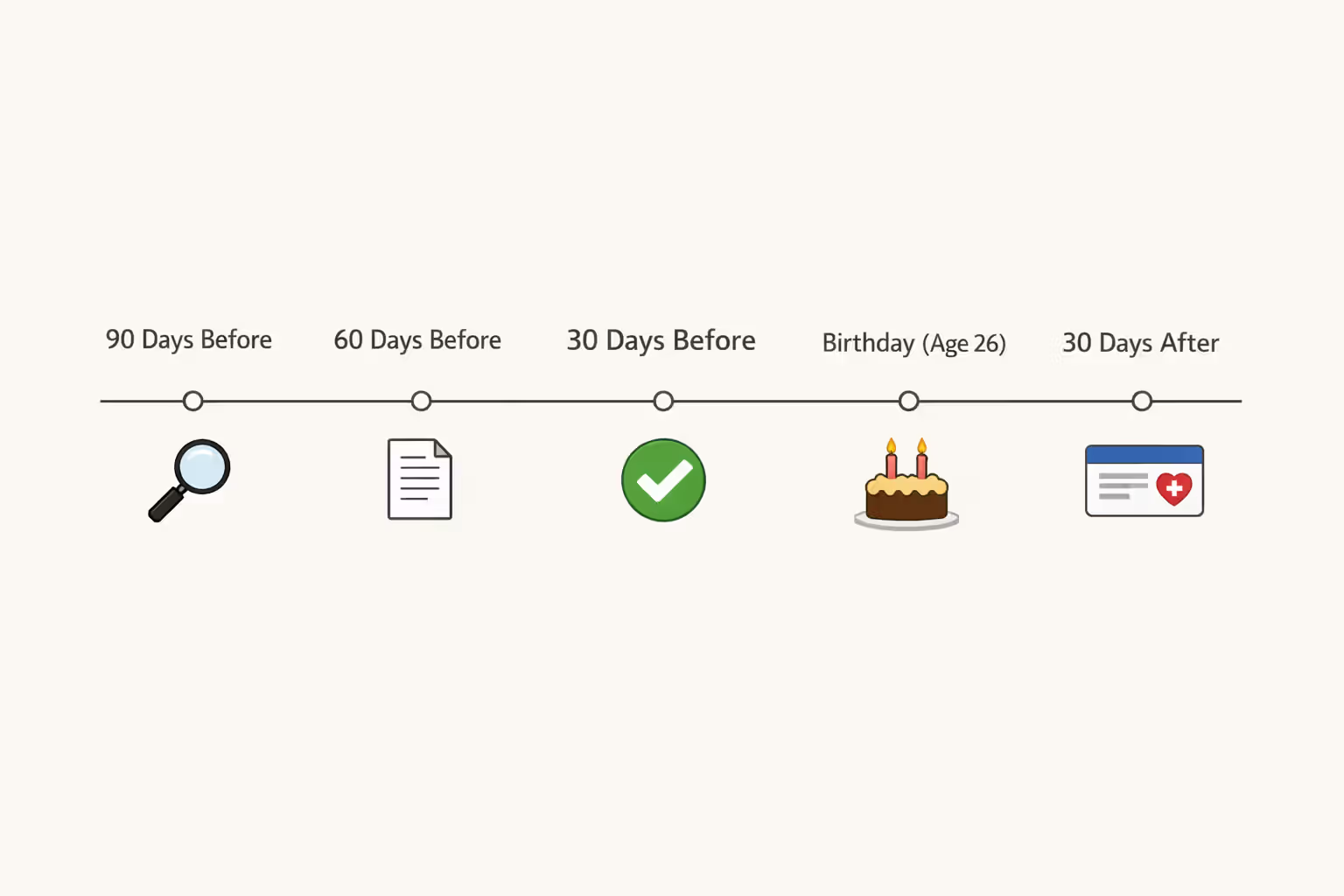
Timeline for transitioning off your parents' plan:
90 days before your 26th birthday: Research alternatives. If you have employer coverage available, ask HR about enrollment procedures. If not, explore marketplace plans and check Medicaid eligibility.
60 days before: Submit enrollment applications. Employer plans typically process special enrollment requests within two weeks. Marketplace applications can take longer if income verification is required.
30 days before: Confirm your new coverage start date aligns with your parent's plan termination date. A gap of even one day can create problems if you need medical care.
Day of your 26th birthday: Your new coverage should be active. Keep both insurance cards for a brief overlap period in case of processing delays.
30 days after: Verify that your first premium payment was processed and coverage is fully active. Test your new insurance card at a pharmacy with a small prescription purchase.
Author: Derek Whitmore;
Source: blaverry.com
Common Mistakes Young Adults Make About Parent Coverage
Many young adults discover coverage issues only when they need medical care—often too late to fix easily.
Assuming automatic notifications: Don't expect your parent's insurance company to remind you about the age-26 cutoff. Some insurers send notices, but many don't. The responsibility falls on you to track your birthday and plan accordingly.
Waiting until the last minute: Starting your insurance search two weeks before your 26th birthday creates unnecessary stress. Applications can take weeks to process, especially marketplace plans that require income verification. Start researching at least three months early.
Not comparing all options: Young adults often grab the first available alternative without comparing costs and coverage. Spend time calculating total annual costs—premiums plus deductibles plus expected out-of-pocket expenses—for each option. The plan with the lowest premium isn't always cheapest overall.
Forgetting about the special enrollment period: Missing the 60-day window around your 26th birthday means waiting months for open enrollment. Set calendar reminders at 90 days, 60 days, and 30 days before your birthday.
Misunderstanding COBRA costs: COBRA sounds appealing until you see the price. Many young adults elect COBRA assuming it costs roughly what their parents paid to add them to the plan, then receive a bill for the full premium amount. Calculate COBRA costs before assuming it's your best option.
Ignoring preventive care deadlines: If you need annual checkups, dental cleanings, or prescription refills, schedule them before your coverage ends. Switching plans mid-year can reset deductibles and out-of-pocket maximums, effectively making you pay twice.
The transition off parental coverage at age 26 is a critical moment when many young adults experience their first coverage gap. Planning ahead—ideally six months before your 26th birthday—dramatically reduces the risk of going uninsured and facing unexpected medical bills
— Jennifer Tolbert
Frequently Asked Questions
The age-26 cutoff for parental health insurance coverage represents a significant milestone in your financial independence. While federal law provides clear eligibility rules, navigating the transition requires advance planning and understanding of your alternatives.
Start researching your options at least three months before your 26th birthday. Compare employer plans, marketplace coverage, and Medicaid eligibility based on total annual costs—not just monthly premiums. Use the special enrollment period wisely, and avoid coverage gaps that could leave you exposed to catastrophic medical bills.
Remember that staying on your parents' plan isn't always the most cost-effective choice. Run the numbers, consider your health needs, and select coverage that balances affordability with adequate protection. The decisions you make during this transition will affect your healthcare access and finances for years to come.










