
Top view of a desk with health insurance documents, calculator, stethoscope, glass jar with coins, and laptop showing financial growth charts
HSA Health Insurance Guide for Beginners
Content
Picking the right health insurance feels like decoding a foreign language sometimes. HSA, HMO, PPO—what do these letters actually mean for your wallet and your family's healthcare?
Here's what makes HSA-eligible plans different: they pair coverage that has you paying more upfront with a savings account that comes with serious tax perks. It's not the perfect fit for everyone, but for certain people, it's borderline brilliant.
Let's walk through how these plans actually function in real life, what they'll cost you, and whether one makes sense for your situation.
What Is HSA Health Insurance?
An HSA-eligible health plan is really two separate pieces working as a team. First, you've got the insurance itself—a high-deductible health plan (HDHP). Second, there's the Health Savings Account, which you can only open if you have that specific type of coverage.
The insurance side requires you to meet a substantial deductible before coverage kicks in. As of 2026, the IRS has set minimum deductibles at $1,650 if you're covering yourself, or $3,300 when insuring your family. Your maximum out-of-pocket spending caps at $8,300 individually or $16,600 for families.
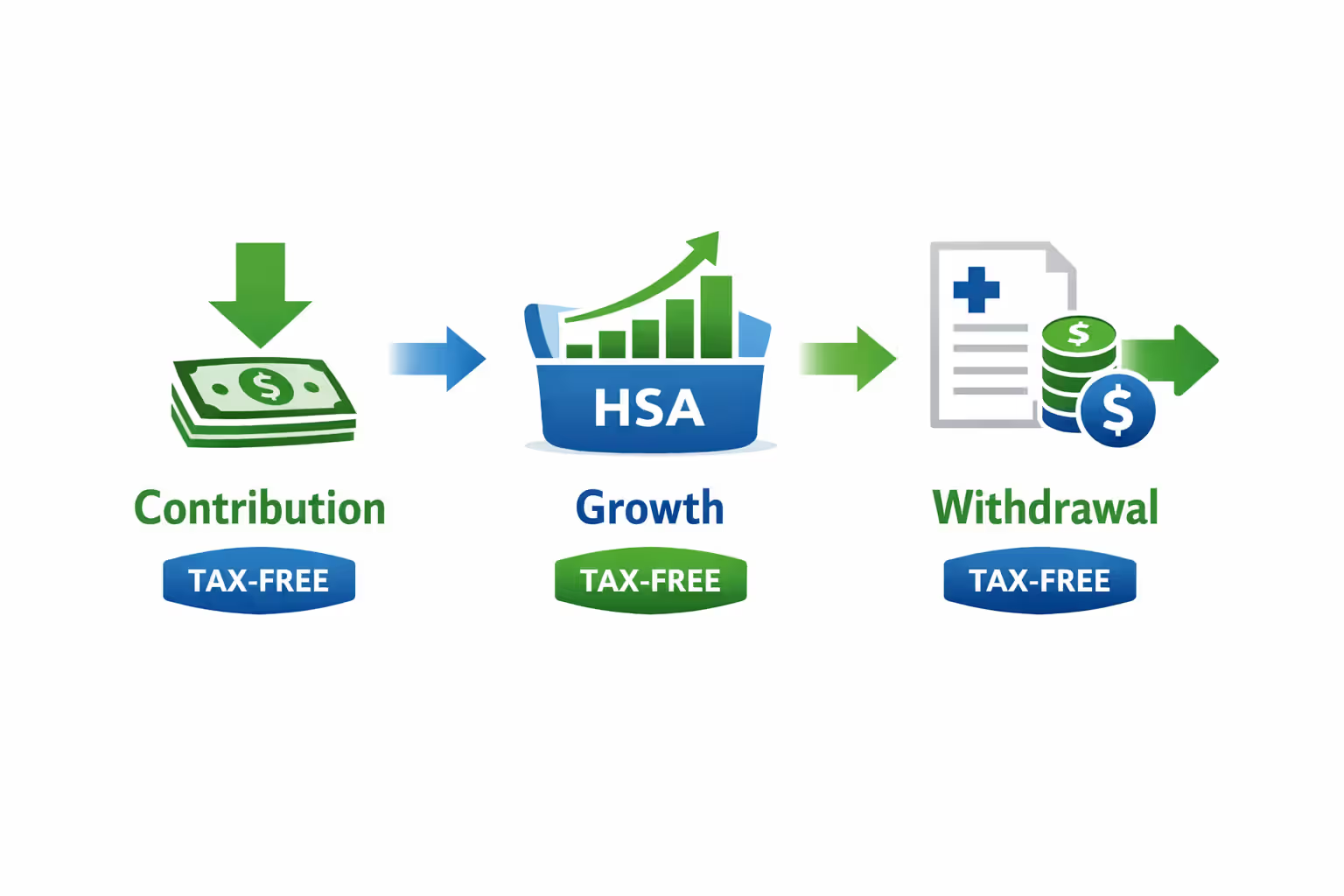
Now for the savings account part. This isn't just another bank account—it's a specialized vehicle where contributions lower your taxable income, the balance grows without tax penalties, and you pull money out tax-free when covering medical bills. That's three separate tax breaks in one account.
Your HSA balance sticks with you forever. Change employers? It's yours. Retire? Still yours. The money rolls over every year, unlike those frustrating Flexible Spending Accounts that make you forfeit unused cash annually.
There's a catch, though. You can't fund an HSA while carrying other non-HDHP coverage, after enrolling in Medicare, or if someone claims you as a dependent on their taxes. The IRS is strict about this—you're either HDHP-only or you're out.
Many people use HSAs strategically. They pay today's medical bills from checking accounts while letting HSA funds grow through investments for decades. Since you can reimburse yourself for old medical expenses anytime (just save those receipts), it functions like a stealth retirement account.
Author: Melissa Grant;
Source: blaverry.com
How Does HSA Health Insurance Work?
Monthly premiums for HDHPs run lower than traditional plans—sometimes $100 to $200 less. But here's the tradeoff: you're covering most healthcare costs from your own pocket until that deductible is satisfied. The silver lining? Preventive services like annual physicals, immunizations, and certain screenings come free regardless of whether you've met your deductible.
Individual coverage lets you set aside $4,300 in 2026, while family plans allow $8,550. Hit 55 years old and you can throw in another $1,000 annually. These caps include every dollar that goes in, whether from your paycheck or your employer's contribution.
Employer matches are common—maybe $500 to $1,500 annually. That's essentially free money padding your healthcare fund. These employer dollars do count against your contribution ceiling, but they still represent guaranteed returns on your healthcare spending.
Funding happens two ways. Payroll deductions reduce your gross income automatically before tax calculations. Or you can deposit money yourself and claim the deduction when filing returns. The tax savings work out identically either way—it's just a timing difference.
What counts as a qualified expense? Doctor appointments, prescriptions, dental work, vision care, therapy sessions, medical devices—the list is extensive. Less obvious items qualify too: acupuncture treatments, chiropractor adjustments, even certain over-the-counter medications.
Here's where strategic thinking pays off: Cover current medical bills from regular income while investing your HSA balance in stocks or mutual funds. Save every medical receipt forever. Twenty years later, you can pull money tax-free from your grown HSA to "reimburse" yourself for expenses you paid decades ago. Meanwhile, that balance has potentially doubled or tripled.
Once you reach 65, the rules shift slightly. Medical expenses still come out tax-free, but you can also withdraw funds for anything else—you'll just pay ordinary income tax like with a traditional IRA. This flexibility transforms HSAs into powerful retirement tools.
HSA vs HMO and PPO Health Insurance Plans
The landscape of health insurance extends beyond just the savings account feature. Structure, costs, and flexibility vary dramatically between plan types.
HSA Health Insurance vs HMO
Health Maintenance Organizations build everything around a primary care doctor who coordinates your care. Need to see a specialist? You'll need a referral first. Step outside the approved network and you're typically paying the entire bill yourself.
HMOs shine at predictability. Maybe you pay $25 for office visits or $10 for generic prescriptions. Budgeting becomes straightforward. The downside? Monthly premiums run higher—often $150 to $300 more than comparable HDHPs.
HSA-qualified plans give you breathing room. No referral requirements for specialists. Many follow PPO-style networks offering both in-network discounts and partial coverage for out-of-network providers. But you're shouldering larger expenses before your deductible kicks in.
Think about payment timing. HMOs spread costs across elevated premiums plus modest per-visit fees. HDHPs slash your monthly bill but make you cover more expenses directly until hitting that deductible threshold. The HSA component, though? That creates tax advantages no HMO can touch.
Picture someone paying $475 monthly for an HMO with a $1,000 deductible, versus $295 monthly for an HDHP carrying a $2,500 deductible. The annual premium gap is $2,160. Contribute that difference to an HSA, face $2,000 in medical costs, and you end up roughly even on spending—but you've banked $450 to $700 in tax savings (depending on your bracket) while building an asset that keeps growing.

Author: Melissa Grant;
Source: blaverry.com
HSA Health Insurance vs PPO
Preferred Provider Organizations split the difference. See any provider without referrals, though staying in-network saves you money. PPOs occupy middle ground between HMOs and HDHPs for both cost structure and freedom.
Typical PPO features include moderate deductibles ($1,000 to $2,500), predictable copays, and coinsurance where you cover a percentage after meeting your deductible. Monthly premiums land between HMO and HDHP rates.
Choosing between PPO and HSA-eligible coverage often hinges on current health status and tax circumstances. PPOs work well when you've got ongoing medical needs and value cost predictability. Managing a chronic condition with regular specialist appointments? Those $35 copays might beat paying full appointment costs while working toward a high deductible.
HSA-eligible plans appeal to folks who can absorb financial ups and downs and want to leverage tax benefits. The ability to contribute pre-tax income, invest that balance, and make tax-free withdrawals for medical expenses generates long-term value that PPOs simply can't replicate.
HSA vs HMO vs PPO: Key Differences at a Glance
| Feature | HSA-Eligible Plan | HMO | PPO |
| Monthly Premium | Lowest option available | Higher costs | Middle-range pricing |
| Deductible | Substantial ($1,650+ solo) | Lower ($500-$1,500 range) | Moderate ($1,000-$2,500 typical) |
| Provider Network | Flexible access, often national | Limited to local network | Flexible, covers in/out of network |
| Referrals Required | No gatekeeping | Primary care doctor manages | No requirements |
| Tax Benefits | Triple tax advantage through HSA | No special tax treatment | No special tax treatment |
| Best For | Generally healthy people, higher earners, long-term planners | Anyone wanting coordinated care with predictable visit costs | Those valuing flexibility with moderate cost certainty |
Who Should Consider HSA Health Insurance?
These plans aren't universal solutions. They excel in specific circumstances while creating headaches in others.
Healthy individuals needing minimal care beyond annual checkups benefit most. Visiting your doctor twice yearly? Paying $300 out-of-pocket for those visits while pocketing $2,400 in annual premium savings creates obvious value. That savings can fund HSA contributions directly, building tax-advantaged wealth.
High earners in the 32% or 37% federal brackets extract substantial returns from HSA contributions. A married couple maxing their family HSA at $8,550 avoids roughly $2,736 to $3,164 in federal taxes alone, before considering state tax savings. These benefits effectively discount their healthcare costs by a third or more.
Retirement-focused individuals increasingly leverage HSAs as supplemental accounts. Unlike 401(k)s or IRAs, HSAs offer tax-free withdrawals for medical expenses at any age. The average 65-year-old couple faces approximately $315,000 in healthcare spending throughout retirement—having a dedicated tax-free fund for this expense category provides real security.
Self-employed people and small business owners extract particular value from HSA contributions, which reduce both income tax and self-employment tax obligations.
But HSA plans aren't appropriate for everyone. Families with young kids making frequent pediatrician visits might find the substantial deductible crushing. Someone managing diabetes, requiring regular specialist care, or taking multiple prescriptions could burn through thousands before their insurance helps meaningfully.
Cash-strapped individuals may struggle with the financial demands. When a $2,500 deductible equals two weeks of income, an unexpected medical event creates genuine hardship that a higher-premium, lower-deductible plan would prevent.
The HSA represents the single most powerful tax-advantaged vehicle available to Americans today. The triple tax benefit—deductible contributions, tax-free growth, and tax-free withdrawals for medical expenses—surpasses even Roth IRAs in efficiency. For individuals who can afford to maximize contributions and allow the balance to compound, an HSA becomes a remarkable wealth-building instrument that addresses one of retirement's most significant expense categories
— Rebecca Walser
Real HSA Health Insurance Examples
Watching how HSA plans function in actual situations clarifies whether they match your circumstances.
Example 1: Young professional building wealth
Marcus, age 28, pulls in $85,000 annually and rarely sees doctors. He enrolled in an HDHP carrying a $1,650 deductible and $320 monthly premium. His previous PPO ran $475 monthly with a $1,200 deductible.
Annual premium savings: $1,860. Marcus dumps $4,300 into his HSA (2026's individual maximum), while his employer kicks in another $500. His total $4,800 contribution slashes his taxable income, saving roughly $1,152 in federal taxes at his 24% bracket.
Marcus visited urgent care once ($125) and got his teeth cleaned ($140), paying both from his HSA. Year-end HSA balance: $4,535. He invests this in a low-fee S&P 500 index fund. After five years of similar results, assuming 7% annual growth, Marcus has accumulated approximately $28,000 in tax-advantaged funds—money he can tap tax-free for medical expenses or let compound for retirement healthcare.

Author: Melissa Grant;
Source: blaverry.com
Example 2: Family with moderate healthcare needs
The Johnsons—parents with two elementary schoolers—selected an HDHP carrying a $3,300 family deductible and $650 monthly premium. Their previous HMO cost $895 monthly with a $1,500 deductible.
Annual premium savings: $2,940. They contribute $7,000 to their HSA, receiving $1,500 from their employer. Medical expenses included routine pediatrician appointments, vaccinations, one emergency room trip for a broken arm ($1,800), and prescription medications ($600).
Total medical spending: $2,400 (preventive care covered at 100%). The ER visit and prescriptions came from their HSA. Despite the higher deductible, they came out ahead: $2,940 in premium savings minus $2,400 in expenses equals $540 net gain, plus they avoided approximately $1,680 in taxes on their $7,000 contribution.
Example 3: Chronic condition management
Sarah, 52, manages rheumatoid arthritis requiring quarterly specialist appointments, routine blood work, and expensive medications. She experimented with switching to an HDHP but quickly discovered it didn't fit her reality.
With a $2,500 deductible, Sarah paid full freight for her $850 monthly biologic medication until satisfying her deductible in March. Specialist visits ($225 each) and lab work ($180 quarterly) accumulated rapidly. By year's end, she'd maxed her $6,500 out-of-pocket limit.
While HSA tax benefits helped somewhat, Sarah found the cash flow demands exhausting and switched back to a PPO with elevated premiums but $40 specialist copays and $50 monthly medication costs after a $1,500 deductible. For her circumstances, predictable expenses trumped tax optimization.
Common HSA Health Insurance Mistakes to Avoid
Even people who benefit from HSA plans sometimes sabotage their own success through avoidable errors.
Draining HSA funds unnecessarily
The costliest mistake is treating your HSA like a checking account and emptying it annually. When you can afford to cover medical expenses from regular income, do exactly that. Allow your HSA balance to grow and compound over decades. Save every single receipt indefinitely—the IRS imposes no time limit on reimbursements, so you can withdraw funds tax-free years later to repay yourself for ancient expenses.
Leaving contribution limits untapped
Plenty of people contribute only what their employer matches, abandoning thousands in tax savings. If you're in the 24% federal bracket and contribute merely $2,000 instead of the $4,300 individual maximum, you're surrendering $552 in annual tax savings. Over 30 years at 7% returns, that difference compounds to approximately $58,000 in lost wealth.
Forcing an HDHP when it doesn't fit
Don't grab an HSA-eligible plan purely for tax benefits when you can't absorb the high deductible comfortably. Someone requiring $8,000 in annual medical care might save $1,600 in taxes but spend an extra $2,500 meeting their deductible compared to a traditional plan. Calculate the numbers for your specific circumstances.
Leaving HSA funds uninvested
Most HSA providers offer investment options once your balance crosses a threshold (commonly $1,000 to $2,000). Leaving substantial balances in low-interest savings accounts squanders growth potential. Treat your HSA like a retirement account and invest in diversified mutual funds or ETFs.
Losing receipts
Document every medical expense you pay out-of-pocket. Decades down the road, you can reimburse yourself tax-free using these receipts, effectively converting your HSA into a traditional IRA with a massive tax-free withdrawal option.
Missing contribution deadlines
You can fund your HSA until the tax filing deadline (usually April 15) for the previous year. Missing this deadline means forfeiting that year's contribution space permanently—you can't make it up later.

Author: Melissa Grant;
Source: blaverry.com
Frequently Asked Questions About HSA Health Insurance
HSA health insurance delivers best results when you grasp both the coverage mechanics and the long-term financial strategy. The combination of reduced premiums, substantial deductibles, and tax-advantaged savings creates distinctive opportunities for appropriate candidates.
If you're relatively healthy, can handle the deductible when necessary, and want to accumulate tax-free wealth for future medical expenses, an HSA-eligible plan deserves serious evaluation. Tax benefits alone can preserve thousands annually, while the long-term compounding potential addresses one of retirement's most significant expense categories.
However, if you've got ongoing medical requirements, limited emergency reserves, or prefer predictable costs over tax optimization, traditional HMO or PPO plans might serve you substantially better. There's no universal "best" choice—only the optimal choice for your specific health profile, financial circumstances, and personal preferences.
Calculate your anticipated medical expenses, compare total annual costs including premiums and out-of-pocket spending, and evaluate your capacity to contribute to and invest HSA funds. The right decision balances immediate healthcare requirements with long-term financial objectives.










